.pdf files to download
Need
Adobe Acrobat Reader to View
Click to Read or Right
Click to Download
George Sheehan M.D. Guru of Running:
Sheehan, G.A., M.D., “Take the Muscles and Run,” Physicians
and Sportsmedicine 9, no. 5 (May1981): 35.
"You might suspect from the emphasis on
cardiopulmonary fitness that the major effect of training is
on the heart and lungs. Guess again. Exercise does nothing
for the lungs; that has been amply proved... Nor does it
especially benefit your heart. Running, no matter what you
have been told, primarily trains and conditions the
muscles."
Interview with Henry A. Solomon M.D.
Author of The Exercise Myth.
Training is no guarantee of health
by Mark Sisson
(www.slowtwitch.com)
Project Total Conditioning
Peterson JA, ATHLETIC JOURNAL Vol. 56 September, 1975
"Contrary to most commonly held beliefs on the subject of
strength training, the training also significantly
improved the cardiovascular condition of the subjects. By
maintaining the intensity of the workouts at a high level
and by limiting the amount of
rest between exercises, the training resulted in improvement
on each of 60 separate
measures of cardiovascular fitness. Contrary to widespread
opinion, not only will a
properly conducted program of strength training produce
increases in muscular strength
but will also significantly improve an individual’s level of
cardiovascular condition. The
data suggests that some of these cardiovascular benefits
apparently cannot be achieved by
any other type of training. "
The Myth of Cardiovascular Health From Exercise
Exercise Doesn’t Prevent heart Disease Peskin BS
Cambridge Institute for Medical Science
Resistance Training to Momentary Muscular Failure Improves
Cardiovascular Fitness in Humans: A Review of Acute
Physiological Responses and Chronic Physiological
Adaptations Steel J et al JEP Online June 2012.
Improved Cardiorespiratory Endurance Following 6
Months of Resistance Exercise in Elderly Men and Women
Vincent KR
et al Arch Intern Med. 2002;162:673-678.
Conclusions Significant improvements in aerobic
capacity and treadmill time to exhaustion can be
obtained in older adults as a consequence of
either high- or low-intensity resistance
exercise. These findings suggest that increased strength, as
a consequence of resistance exercise training, may
allow older adults to reach and/or improve their
aerobic capacity.
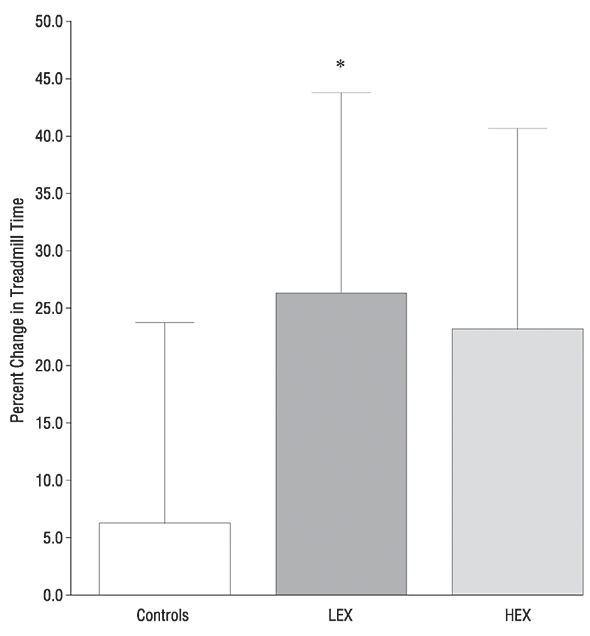
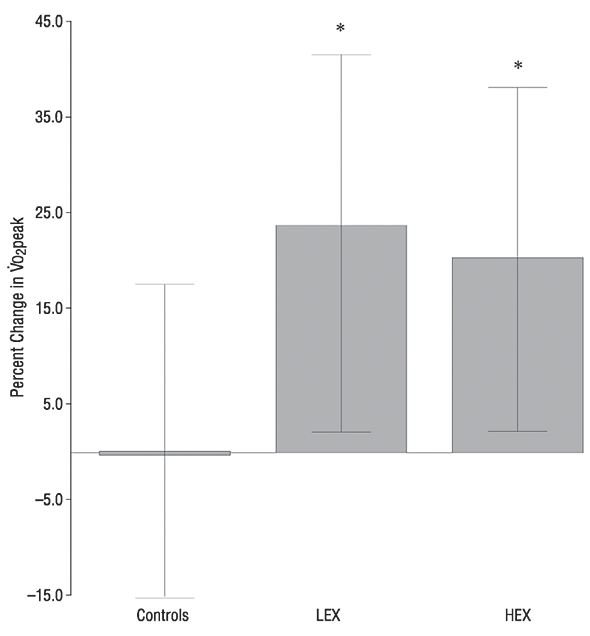
Effect of Exercise Training on Peak Aerobic
Power, Left Ventricular Morphology, and Muscle Strength in
Healthy Older Women Haykowsky M et al The Journals
of Gerontology Series A: Biological Sciences and Medical
Sciences 60:307-311 (2005)
The mechanism responsible for the improvement in VO2peak,
in healthy older women has received minimal
attention. The few studies performed to date (24–26)
have focused on aerobic based exercise
interventions. Overall, the findings of these
studies suggest that the increase in VO2peak
associated with AT is due to the improvement in
peak arteriovenous oxygen difference, as no
significant change was found for heart rate (24,25),
end diastolic volume (24),
end systolic volume (24),
stroke volume (24,25),
ejection fraction (24,26),
or cardiac output during peak exercise (24,25).
Lastly, our finding of no favorable
cardiac adaptations after AT, ST, or COMT
indicates that the increase in VO2peak was likely
due to improvements in skeletal muscle function
and morphology. More specifically, a number of
investigators have found that AT and/or ST is
associated with an increase in skeletal muscle
fiber cross-sectional area (8,9,30),
capillary density (9,30),
capillary-to-fiber ratio (8,9,30),
and oxidative enzyme activity (8,30)
in older men and women.
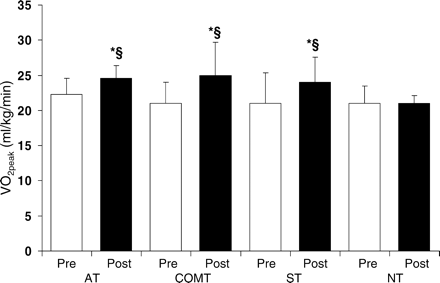
Resistance and aerobic training in older men:
effects on
 O2
peak and the capillary supply to
skeletal muscle Hepple et al
J Appl Physiol 82:
1305-1310, 1997;
O2
peak and the capillary supply to
skeletal muscle Hepple et al
J Appl Physiol 82:
1305-1310, 1997;
We observed that a program of 9 wk of RT followed
by 9 wk of AT produced a similar increase in
 O2
peak (l/min) as did 18 wk of AT in a
population of older men. In conjunction with the
changes in
O2
peak (l/min) as did 18 wk of AT in a
population of older men. In conjunction with the
changes in
 O2
peak, we observed significant increases in the
capillary-to-fiber surface interface (as reflected in
an increased CFPE index) after both RT and AT,
whereas the CD was significantly increased only
after AT. When the
O2
peak, we observed significant increases in the
capillary-to-fiber surface interface (as reflected in
an increased CFPE index) after both RT and AT,
whereas the CD was significantly increased only
after AT. When the
 O2
peak was regressed as a function of the
capillary supply, the CFPE index was found to
explain a greater proportion of the variance in
O2
peak was regressed as a function of the
capillary supply, the CFPE index was found to
explain a greater proportion of the variance in
 O2
peak than did the other indexes of the
capillary supply. These observations support the
utility of the CFPE index in providing an indication
of the capacity for oxygen flux between the
capillaries and muscle fibers and support an
important role for the capillaries in the
O2
peak than did the other indexes of the
capillary supply. These observations support the
utility of the CFPE index in providing an indication
of the capacity for oxygen flux between the
capillaries and muscle fibers and support an
important role for the capillaries in the
 O2
peak response in the older population. They also
suggest the possibility that high-intensity RT
and AT, by increasing the capillary supply to the
skeletal muscle fibers, may operate through
similar mechanisms to increase the
O2
peak response in the older population. They also
suggest the possibility that high-intensity RT
and AT, by increasing the capillary supply to the
skeletal muscle fibers, may operate through
similar mechanisms to increase the
 O2
peak in the older population
O2
peak in the older population
Strength training and determinants of VO2max
in older men
Frontera WR et al J Appl Physiol 68: 329-333,
1990;
US Department of Agriculture Human
Nutrition Research Center on Aging, Tufts University,
Boston, Massachusetts
Large energetic adaptations of elderly muscle
to resistance and endurance training
Jubrias SA et al J Appl
Physiol 90: 1663-1670, 2001;
RT and oxidative properties. The increase in kPCr
and oxidative capacity in the RT group was unexpected. RT in
young subjects typically results in lower
oxidative enzyme activity and Vv(mt,f), reflecting the
dilution of mitochondrial structure with the
increase in muscle size (9,
36, 37). Our RT
subjects had greater muscle size after training,
but this did not lead to a reduction in Vv(mt,f) or
oxidative properties. Instead, we found an
increased oxidative capacity, and this increase
(50%) was greater than that found for the ET
group. In addition, Vv(mt,f) increased after RT, in contrast
to the lack of change after ET. These
improvements in oxidative properties for the RT
group are supported by previous reports of increased
oxidative enzyme activity and capillary-to-fiber ratio
after RT in the elderly (18,
22, 23). Our results
indicate that elderly muscle shows adaptations in
muscle size and strength in common with young
muscle after RT, but the increase in oxidative properties
is an unexpected response of elderly muscle to this
training
Effects of exercise training on
thermoregulatory responses and blood volume in older men
Okazaki, K et al J
Appl Physiol 93: 1630-1637, 2002.
Resistance versus endurance training in patients with
COPD and peripheral muscle weakness Spruit MA et al Eur
Respir J 2002; 19:1072-1078
Randomized trial of progressive resistance
training to counteract the myopathy of chronic heart failure
Pu CT et al J Appl
Physiol 90: 2341-2350, 2001;
Effects of High-Intensity Interval Walking
Training on Physical Fitness and Blood Pressure in
Middle-Aged and Older People Nemeto k et al
Mayo Clinic Proceedings
July 2007 vol. 82
no. 7
803-811
Exercise: A Walk in the Park? Levine J
Mayo Clinic Proceedings
July 2007 vol. 82
no. 7
797-798
Progressive Resistance Exercise in Physical
Therapy: A Summary of Systematic Reviews Taylor NF
PHYS THER
Vol. 85, No. 11, November 2005, pp. 1208-1223
Skeletal Muscle and Cardiovascular Adaptations to
Exercise Conditioning in Older Coronary Patients
Ades et al Circulation, August 1, 1996; 94(3):
323 - 330.
Accordingly, in the present study, we tested the
hypothesis that conditioning-induced adaptations
in older coronary patients are primarily noncardiovascular
in nature. If true, this may have implications
regarding optimal training techniques in this
group of patients.
Conclusions Older coronary patients successfully
improve peak aerobic capacity after 3 and 12
months of supervised aerobic conditioning
compared with control subjects. The mechanism of
the increase in peak aerobic capacity is
associated almost exclusively with peripheral
skeletal muscle adaptations, with no discernible
improvements in cardiac output or calf blood flow.
Table 2. Cardiac Response to Exercise
Conditioning
| |
Baseline
(n=55) |
3 mo
(n=55) |
Baseline
(n=21) |
12 mo
(n=21) |
|
| Peak
workload, W |
83±32 |
93±28 (P<.001) |
84±29 |
97±28 (P<.001) |
| Resting
heart rate, bpm |
72±13 |
68±13 (P=.001) |
74±13 |
67±10 (P=.02) |
| Peak heart
rate, bpm |
119±21 |
121±23 |
118±27 |
115±20 |
| Resting EF,
% |
51±11 |
51±11 |
51±13 |
52±11 |
| Peak EF, % |
55±13 |
57±12 (P=.07) |
55±12 |
52±14 |
| Peak
end-diastolic volume, mL |
197±85 |
181±73 (P=.07) |
209±79 |
204±81 |
| Peak
end-systolic volume, mL |
91±59 |
82±46 (P=.06) |
93±54 |
95±51 |
| Peak
stroke volume, mL |
108±47 |
99±42 |
116±51 |
109±44 |
| Peak
cardiac output, L/min |
12.6±5.8 |
11.7±5.6 |
13.8±6.7 |
11.8±2.8 |
|

"Sarcopenia and Dynapenia" Clark et al J.
Gerontology 2008 63:8: 829-834
